Explore the Possible Root Causes
Understanding chronic fatigue and low cellular energy often requires looking deeper than standard tests.
Many biological systems contribute to how the body produces and uses energy.
This page explores several areas researchers and clinicians are investigating when fatigue, brain fog, and exercise intolerance persist.
Potential Root Causes
Chronic fatigue and persistent low energy are rarely caused by a single problem.
In many cases, multiple biological systems may be involved in how the body produces and uses energy.
Researchers studying fatigue and mitochondrial function often look at interactions between the immune system, environmental exposures, nutrition, hormones, and nervous system regulation.
The diagram below illustrates several of the major areas that may influence cellular energy production.
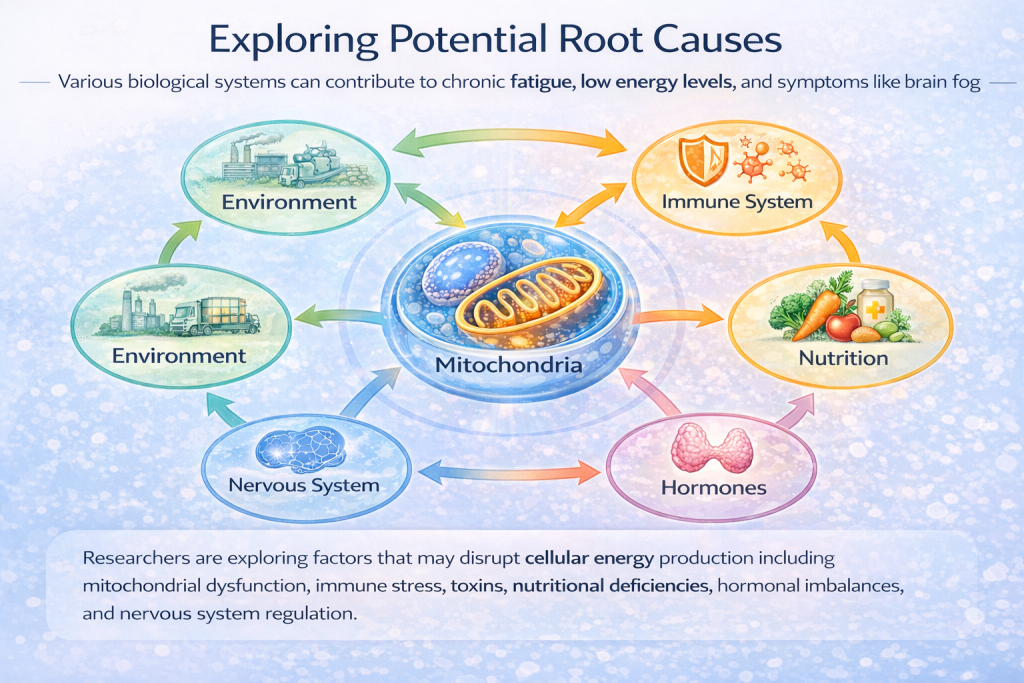
How multiple biological systems can influence cellular energy.
Many factors can interact to affect how the body produces and uses energy.
This diagram highlights several areas researchers are exploring when investigating chronic fatigue and mitochondrial dysfunction.
Each of the areas shown above is explored in more detail below.
Mitochondrial Dysfunction

Illustration of mitochondrial stress and oxidative damage affecting cellular energy production.
Mitochondria are responsible for producing ATP — the primary energy molecule used by cells.
When mitochondria are not functioning efficiently, cells may struggle to generate enough energy to support normal body activity.
Researchers studying mitochondrial dysfunction often examine factors such as:
• impaired ATP production
• oxidative stress
• mitochondrial DNA damage
• reduced cellular energy metabolism
Because mitochondria exist in nearly every cell in the body, disruptions can affect multiple systems including the brain, muscles, and immune system.
Immune System Stress

Illustration of immune system activation and the biological stress response that can increase the body’s overall energy demand.
The immune system requires large amounts of energy to function properly.
When the immune system remains activated for long periods of time, it can place a significant demand on the body’s energy resources.
Possible contributors may include:
• chronic inflammation
• viral or bacterial infections
• immune dysregulation
• autoimmune responses
In some cases, the body may remain in a prolonged state of immune activation long after the initial trigger has passed.
Environmental Exposures

An illustration depicting potential environmental exposures such as industrial pollutants, chemical solvents, and airborne contaminants that may contribute to biological stress.
Certain environmental exposures may place stress on cellular energy systems.
Researchers have investigated links between long-term exposure and mitochondrial stress.
Examples sometimes discussed in research include:
• toxic chemicals
• heavy metals
• environmental pollutants
• military-related exposures
Understanding the long-term biological effects of these exposures is an active area of research.
Nutritional Deficiencies

An illustration depicting foods and nutrients that support cellular energy production. Deficiencies in key vitamins, minerals, and amino acids may reduce the body’s ability to efficiently produce cellular energy.
Cells require specific nutrients to support energy production pathways.
Deficiencies in key nutrients may reduce the body’s ability to produce ATP efficiently.
Important nutrients often studied include:
• B vitamins
• magnesium
• amino acids
• carnitine
• antioxidants
These nutrients play roles in mitochondrial function and cellular metabolism.
Hormonal and Metabolic Factures
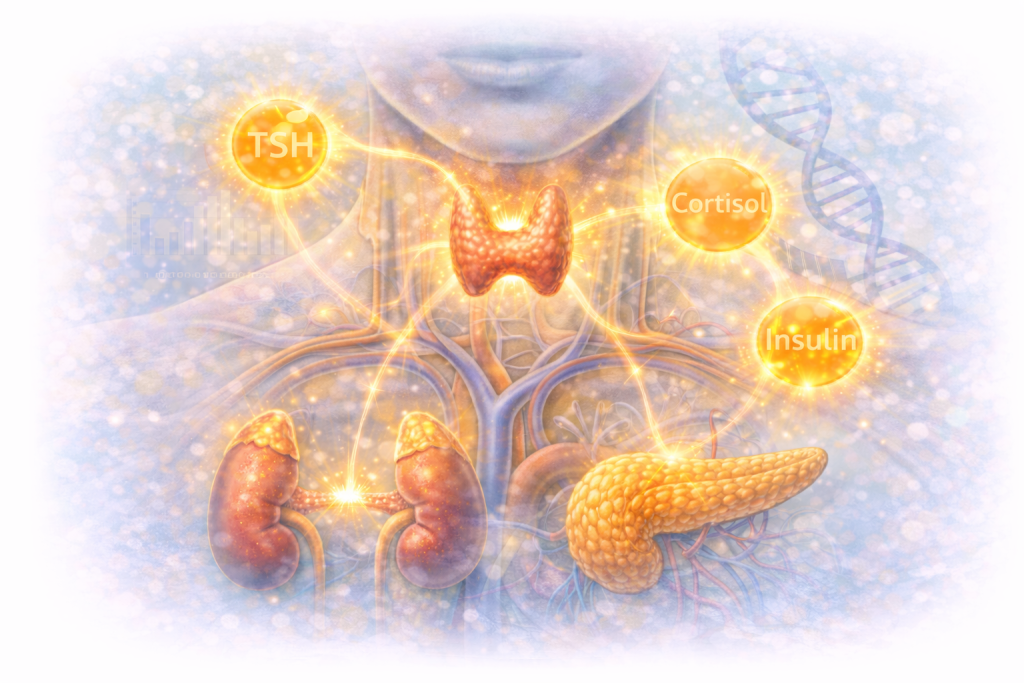
An illustration depicting endocrine glands and hormones involved in metabolic regulation. Disruptions in hormonal signaling—such as thyroid function, cortisol regulation, and insulin balance—may influence cellular energy and overall metabolism.
Hormones help regulate many of the body’s energy systems.
Disruptions in hormonal balance may affect metabolism, sleep, recovery, and overall energy levels.
Researchers sometimes explore connections involving:
• thyroid function
• adrenal regulation
• insulin sensitivity
• metabolic signaling pathways
Nervous System Regulation
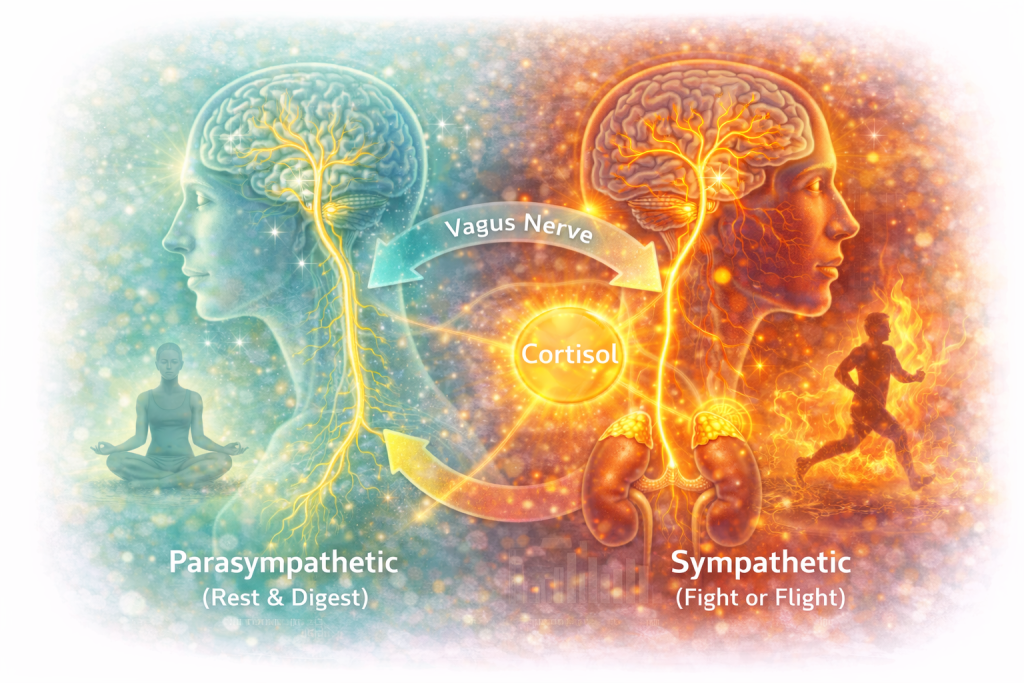
An illustration depicting the autonomic nervous system, including the balance between parasympathetic “rest and digest” activity and sympathetic “fight or flight” responses. Prolonged stress activation may influence hormonal signaling, inflammation, and the body’s overall energy regulation.
The nervous system also influences how energy is distributed and used throughout the body.
When the nervous system is under prolonged stress, it may affect sleep, recovery, and the body’s ability to maintain stable energy levels.
Areas being studied include:
• autonomic nervous system balance
• chronic stress responses
• sleep disruption
• nervous system overactivation
Why Root Causes are Complex
In many cases, fatigue does not come from a single cause.
Instead, multiple systems may be interacting at the same time.
For example:
• mitochondrial stress
• immune activation
• environmental exposures
• nutritional deficiencies
These overlapping factors can make fatigue difficult to diagnose through standard testing alone.
Understanding the broader biological picture can help guide further investigation.
Where to go Next
If you’re exploring these topics for the first time, the next step is to understand the practical approaches people are using to support cellular energy.